- Clinical Study
- Relationships between Thigh and Waist Circumference, Hemoglobin Glycation Index, and Carotid Plaque in Patients with Type 2 Diabetes
-
Myung Ki Yoon, Jun Goo Kang, Seong Jin Lee, Sung-Hee Ihm, Kap Bum Huh, Chul Sik Kim
-
Endocrinol Metab. 2020;35(2):319-328. Published online June 24, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.2.319
-
-
8,369
View
-
145
Download
-
4
Web of Science
-
3
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
This study investigated the relationships of thigh and waist circumference with the hemoglobin glycation index (HGI) and carotid atherosclerosis in patients with type 2 diabetes.
Methods
This observational study included 3,075 Korean patients with type 2 diabetes, in whom anthropometric measurements and carotid ultrasonography were conducted. HGI was defined as the measured hemoglobin A1c (HbA1c) level minus the predicted HbA1c level, which was calculated using the linear relationship between HbA1c and fasting plasma glucose levels. Carotid atherosclerosis was defined as a clearly isolated focal plaque or focal wall thickening >50% of the surrounding intima-media thickness.
Results
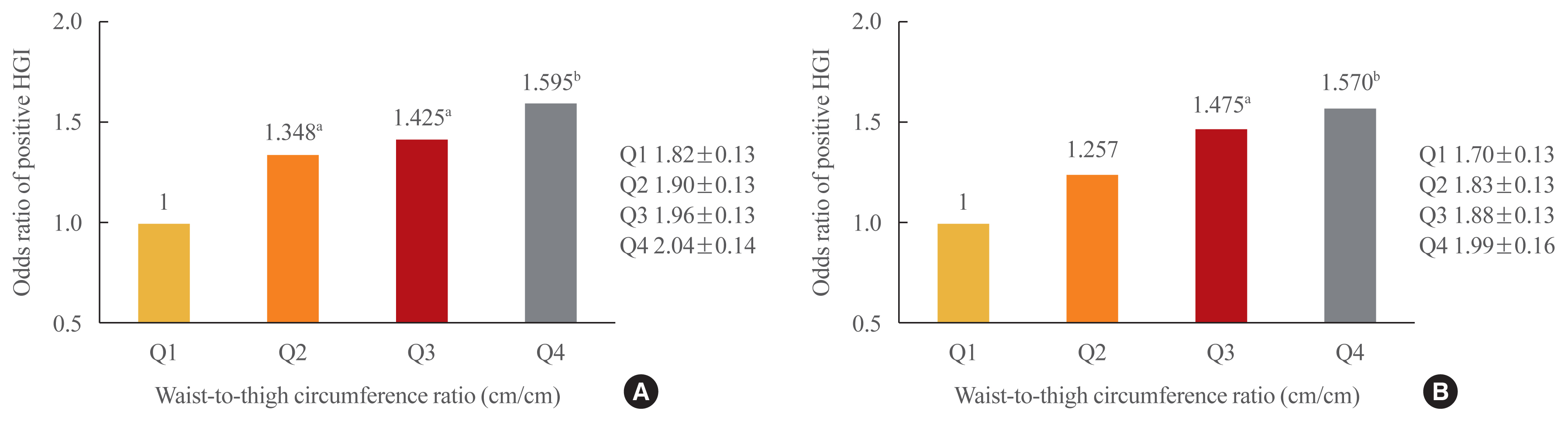
The frequency of a positive HGI decreased with increasing thigh circumference in men and increased with increasing waist circumference in women after adjusting for potential confounding variables. Thigh and waist circumference had a combined augmentative effect on the likelihood of positive HGI, which was dramatically higher in patients in higher waist-to-thigh ratio quartiles (adjusted odds ratios for the highest compared to the lowest quartile: 1.595 in men and 1.570 in women). Additionally, the larger the thigh circumference, the lower the risk of carotid atherosclerosis, although in women, this relationship lacked significance after adjustment for potential confounders.
Conclusion
HGI was associated with thigh circumference in men and waist circumference in women. In addition, the combination of low thigh circumference and high waist circumference was strongly associated with a higher HGI in Korean patients with type 2 diabetes. In particular, thigh circumference was associated with carotid atherosclerosis in men. However, further longitudinal studies are warranted.
-
Citations
Citations to this article as recorded by  - Association between hemoglobin glycation index and subclinical myocardial injury in the general population free from cardiovascular disease
Zhenwei Wang, Yihai Liu, Jing Xie, Nai-Feng Liu
Nutrition, Metabolism and Cardiovascular Diseases.2022; 32(2): 469. CrossRef - Association of Hemoglobin Glycation Index With Contrast-Induced Acute Kidney Injury in Patients Undergoing Coronary Angiography: A Retrospective Study
Zhezhe Chen, Duanbin Li, Maoning Lin, Hangpan Jiang, Tian Xu, Yu Shan, Guosheng Fu, Min Wang, Wenbin Zhang
Frontiers in Physiology.2022;[Epub] CrossRef - Associations of continuous glucose monitoring-assessed glucose variability with intima-media thickness and ultrasonic tissue characteristics of the carotid arteries: a cross-sectional analysis in patients with type 2 diabetes
Naohiro Taya, Naoto Katakami, Tomoya Mita, Yosuke Okada, Satomi Wakasugi, Hidenori Yoshii, Toshihiko Shiraiwa, Akihito Otsuka, Yutaka Umayahara, Kayoko Ryomoto, Masahiro Hatazaki, Tetsuyuki Yasuda, Tsunehiko Yamamoto, Masahiko Gosho, Iichiro Shimomura, Hi
Cardiovascular Diabetology.2021;[Epub] CrossRef
- Impact of Serum Adiponectin Concentration on Progression of Carotid Atherosclerosis in Patients with Type 2 Diabetes Mellitus.
-
Chul Sik Kim, Ju Ri Park, Sung Hoon Yu, Jun Goo Kang, Ohk Hyun Ryu, Seong Jin Lee, Eun Gyung Hong, Doo Man Kim, Jae Myung Yoo, Sung Hee Ihm, Moon Gi Choi, Hyung Joon Yoo
-
Endocrinol Metab. 2012;27(1):31-38. Published online March 1, 2012
-
DOI: https://doi.org/10.3803/EnM.2012.27.1.31
-
-
 Abstract Abstract
 PDF PDF
- BACKGROUND
Increased cardiovascular events, which is the leading cause of death in type 2 diabetic patients, are mainly caused by accelerated atherosclerosis. Adiponectin has been suggested as a risk factor for cardiovascular diseases in cross-sectional studies. However, little is known about the impact of adiponectin on the progression of carotid atherosclerosis in type 2 diabetic patients. This study was conducted to evaluate the impact of early adiponectin levels on the progression of carotid atherosclerosis. METHODS: From March 2009, 150 patients with type 2 diabetes were consecutively enrolled in our affiliated outpatient clinic. Anthropometric and biochemical data, including adiponectin levels, were measured in each participant. We measured the carotid intima-media thickness (CIMT) at baseline and at 1-year follow-up (n = 111). Then, we prospectively studied the relationship between the serum adiponectin levels and the progression of CIMT for 1 year. RESULTS: Adiponectin levels negatively correlated with CIMT (r = -0.219, P = 0.015). Moreover, mean progression of CIMT was 0.016 +/- 0.040 mm. However, there was no correlation between adiponectin levels and the progression of CIMT within 1-year follow-up period (r = -0.156, P = 0.080). Age (beta = 0.556, P = 0.004), LDL cholesterol (beta = 0.276, P = 0.042), and A1C (beta = 0.309, P = 0.038) were found to be independent risk factors for CIMT. However, A1C (beta = 0.311, P = 0.042) was found to be the only independent risk factor for the progression of CIMT. CONCLUSION: In our study, adiponectin levels were negatively associated with CIMT. However, it did not affect the progression of CIMT at 1-year follow-up. Overall glycemic control is the most important factor in the progression of CIMT in patients with type 2 diabetes.
- A Case of Thyrotoxic Periodic Paralysis with Rhabdomyolysis.
-
Seo Hee Lee, Seong Yeol Kim, Hae Ri Lee, Jun Goo Kang, Ohk Hyun Ryu, Chul Sik Kim, Byung Wan Lee, Seong Jin Lee, Eun Gyoung Hong, Hyeon Kyu Kim, Doo Man Kim, Jae Myung Yu, Sung Hee Ihm, Moon Gi Choi, Hyung Joon Yoo
-
J Korean Endocr Soc. 2008;23(6):425-429. Published online December 1, 2008
-
DOI: https://doi.org/10.3803/jkes.2008.23.6.425
-
-
 Abstract Abstract
 PDF PDF
- Hyperthyroidism combined with rhabdomyolysis is extremely rare. There are only 6 reported cases of hyperthyroidism accompanied with rhabdomyolysis in the medical literature. Rhabdomyolysis is a syndrome involving the breakdown of skeletal muscle, and this causes myoglobin and intracellular protein to leak into the circulation. The causes of rhabdomyolysis include trauma, electrolyte abnormality, infection, drug, toxin and hypothyroidism. We report here on a patient who presented with thyrotoxic periodic paralysis and rhabdomyolysis with hypokalemia. He complained of lower leg paralysis along with muscle tenderness, and the laboratory findings showed elevated creatine kinase (CK) levels. After treatment by hydration, potassium replacement and drug medication, including propylthiouracil and beta-blocker, his CK levels were normalized and his symptoms were much improved. For patient with thyrotoxic periodic paralysis and muscle tenderness, the possibility of rhabdomyolysis should be clarified by examining the CK levels.
- A Case of Unilateral Exophthalmos Caused by a Dural Arteriovenous Malformation in Thyroid-Associated Ophthalmopathy.
-
Sun Ryoung Choi, Seong Jin Lee, Hae Ri Lee, Jun Goo Kang, Ohk Hyun Ryu, Chul Sik Kim, Byung Wan Lee, Eun Gyung Hong, Hyeon Kyu Kim, Doo Man Kim, Jae Myung Yoo, Sung Hee Ihm, Moon Gi Choi, Hyung Joon Yoo
-
J Korean Endocr Soc. 2008;23(1):51-55. Published online February 1, 2008
-
DOI: https://doi.org/10.3803/jkes.2008.23.1.51
-
-
1,974
View
-
20
Download
-
2
Crossref
-
 Abstract Abstract
 PDF PDF
- Thyroid-associated ophthalmopathy is associated with thyroid dysfunction, particularly Graves' disease, and is manifested as eye signs, including proptosis. In cases of unilateral exophthalmos with thyroid-associated ophthalmopathy, other causes such as orbital neoplasm, carotid-cavernous fistula, cavernous sinus thrombosis, and dural arteriovenous malformation (AVM) should be excluded. Dural AVM, an abnormal dural arteriovenous connection, is a rare neurovascular entity that mimics thyroid-associated ophthalmopathy. When eye involvement is unilateral or asymmetric, dural AVM can be considered in the differential diagnosis of thyroid-associated ophthalmopathy. A twenty-six year-old woman presented with unilateral exophthalmos in Graves' disease. By orbital magnetic resonance imaging and cerebral angiography, thyroid-associated ophthalmopathy and dural AVM were diagnosed. The unilateral exophthalmos improved after coil embolization of the dural AVM. In summary, we report the first case of a dural AVM with Graves' disease and thyroid-associated ophthalmopathy.
-
Citations
Citations to this article as recorded by  - Proptosis as a Primary Symptom of Brain Arteriovenous Malformation
Jong Eun Lee, Jin Sook Yoon, Keun Young Park
Ophthalmic Plastic & Reconstructive Surgery.2020; 36(2): e53. CrossRef - Ophthalmopathy Induced by Bilateral Carotid Cavernous Fistula in a Patient with Graves' Disease
Jong Kun Ha, Ji Hye Suk, A Ra Jo, Chan Woo Jung, Bong Jae Kim, Seong Oh Park, Sang Su Kim, Mi Kyung Kim
Endocrinology and Metabolism.2011; 26(4): 335. CrossRef
- The Clinical Significance of Retinoic Acid Receptor beta Expressions in Primary and Recurred Metastatic Lymph Node Papillary Thyroid Carcinomas.
-
Jae Pil Han, Seong Jin Lee, Kyung Chan Choi, Young Euy Park, Hae Ri Lee, Jun Goo Kang, Ohk Hyun Ryu, Chul Sik Kim, Byung Wan Lee, Eun Gyung Hong, Hyeon Kyu Kim, Doo Man Kim, Jae Myung Yoo, Sung Hee Ihm, Hyung Joon Yoo, Moon Gi Choi
-
J Korean Endocr Soc. 2007;22(6):419-427. Published online December 1, 2007
-
DOI: https://doi.org/10.3803/jkes.2007.22.6.419
-
-
 Abstract Abstract
 PDF PDF
- BACKGROUND
The present study was designed to investigate the correlations of retinoic acid receptor beta(RARbeta) expression for primary and recurred metastatic lymph node (LN) papillary thyroid carcinoma (PTC) tissues and the correlations of RARbeta expression with the uptake of I(131) as detected on a whole body scan (WBS). METHODS: Primary and metastatic LN PTC tissues were examined by immunohistochemical methods. Staining positivity was calculated, and staining intensity was graded as negative (0), weak (1+), moderate (2+) and strong (3+). Nuclear staining intensity (NSI) of cells from tissues was also examined. RESULTS: Seventeen patients who had regional cervical LN metastasis without distant metastasis were included in the study, and 13 patients had the abnormal uptake of I(131) as detected on a WBS. In primary PTC tissues, RARbeta staining positivity and intensity of carcinoma cells were significantly higher than those of normal cells but NSI was significantly higher in normal cells than carcinoma cells. Between primary and metastatic LN PTC tissues, RARbeta staining intensity was correlated after controlling for age. Primary PTC tissues from 14 (82.4%) out of 17 patients were concordant between NSI and the uptake of I(131) as detected on a WBS. NSI predicted the I(131) uptake as detected on a WBS with 81.3% positive predicted value (PPV) and 100% negative predicted value. Metastatic LN PTC tissues from 13 (76.5%) out of 17 patients were concordant between NSI and the uptake of I(131) as detected on a WBS. NSI predicted the uptake of I(131) as detected on a WBS with 76.5% PPV. When the results of NSI taken either as positive or negative were correlated with those of the uptake of I(131) as detected on a WBS in primary and metastatic LN PTC tissues, the correlation was not significant after controlling for age. CONCLUSION: Our results demonstrate that nuclear RARbeta expression may be decreased in PTC tissues than normal thyroid tissues, and RARbeta expression in primary PTC tissues as well as in recurred metastatic LN PTC tissues may predict the uptake of I(131) as detected on a WBS.
- A Case of Patient with Opioid-Induced Adrenocortical Insufficiency and Hypogonadism.
-
Hai Jin Kim, Chul Sik Kim, Jong Suk Park, Jina Park, Eun Seok Kang, Chul Woo Ahn, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee
-
J Korean Endocr Soc. 2006;21(3):257-260. Published online June 1, 2006
-
DOI: https://doi.org/10.3803/jkes.2006.21.3.257
-
-
 Abstract Abstract
 PDF PDF
- Opioids are known to decrease plasma cortisol and testosterone level in human and other mammals. Nowadays, opioid use is exponentially increasing, but little is known about its side effects. With the help of progressive human science, we can habit longer life and as result, are becoming more avid for healthy life. In this respect, analgesics play important role in maintaining good and healthy quality of life. For this reason, it is important to fully understand its side effects and handle it with special precaution. We are reporting a 22-year-old male who had been taken opioid analgesic for more than six years to relieve chronic, intractable headache. Then, his hormone test revealed hypogonadotropic hypogonadism combined with hypoadrenocorticotropic hypoadrenalism but showed no definite clinical features except for sexual frigidity. After two years of oxycodon discontinuation, we reevaluated that his hormone test, and all other laboratory tests returned to the normal range.
- Reversible Pituitary Dysfunction in a Patient with Cushing's Syndrome due to Adrenal Adenoma.
-
Jee Hyun Kong, Kyung Wook Kim, Hei Jin Kim, Ji Sun Nam, Jin A Park, Jong Sook Park, Chul Sik Kim, Byung Soo Moon, Soon Won Hong, Chul Woo Ahn, Kyung Rae Kim
-
J Korean Endocr Soc. 2006;21(2):146-152. Published online April 1, 2006
-
DOI: https://doi.org/10.3803/jkes.2006.21.2.146
-
-
 Abstract Abstract
 PDF PDF
- A 45-year-old woman who complained of weight gain and irregular menstruation was diagnosed as having Cushing's syndrome due to a 3 cm sized left adrenal adenoma. She underwent left adrenalectomy, and she also underwent combined anterior pituitary tests before and 9 months after the surgery. The growth hormone and adrenocorticotropic hormone levels failed to respond to hypoglycemia before the surgery, but their responses recovered after the surgery. Cortisol and thyroid stimulating hormone failed to respond to hypoglycemia and thyrotropin releasing hormone (TRH) before the surgery, respectively, but these were improved after the surgery. Luteinizing hormone, follicle stimulating hormone, and prolactin adequately responded to gonadotropin-releasing hormone and TRH, respectively, before and after the surgery. However, the basal levels of these hormones were higher after adrenalectomy, suggesting that hypercortisolemia had a significant influence on all the pituitary hormones.
- A Case of Multiple Endocrine Neoplasia Type 1 with Papillary Thyroid Carcinoma.
-
Hai Jin Kim, Chul Sik Kim, Hyun Chul Je, Jina Park, Jong Suk Park, Jee Hyun Kong, Eun Seok Kang, Chul Woo Ahn, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee, Hang Suk Jang, Soon Won Hong
-
J Korean Endocr Soc. 2006;21(1):79-84. Published online February 1, 2006
-
DOI: https://doi.org/10.3803/jkes.2006.21.1.79
-
-
1,809
View
-
21
Download
-
1
Crossref
-
 Abstract Abstract
 PDF PDF
- This is the first report of papillary thyroid carcinoma combined with multiple endocrine neoplasia type 1 (MEN 1). It is an hereditary syndrome characterized by neoplastic disorders such as pituitary adenoma, parathyroid adenoma or hyperplasia and pancreatic neuroendocrine tumor, such as gastrinoma just like in our case. But sometimes pheochromocytoma, mucosal ganglioneuromas, lipoma, forgut carcinoid and thyroid disease could be accompany the disease, but coincidental papillary thyroid carcinoma was never reported before in Korea. Herein we represent a 39-year-old woman who manifested typical features of MEN 1 with coincidental papillary thyroid carcinoma. Despite with definite family history of MEN 1, her genetic analysis of DNA had not found any germline mutation in MEN 1 gene. Unidentified culprit gene unable further genetic study of finding LOH (loss of heterogeneity) in 11q13, the possible explanation of papillary thyroid carcinoma as a new component of MEN 1. As we have experienced a case of MEN 1 combined with papillary thyroid carcinoma, we report it with the review of literature.
-
Citations
Citations to this article as recorded by  - A Case of Multiple Endocrine Neoplasia Type I with Atypical Clinical Course
Yun Sun Choi, Youn Sun Bai, Bon Jeong Ku, Young Suk Jo, Young Kun Kim, Heung Kyu Ro, Minho Shong
Journal of Korean Endocrine Society.2008; 23(4): 266. CrossRef
- A Case of Acromegaly Caused by Double Pituitary Adenomas.
-
Hai Jin Kim, Chul Sik Kim, Jong Suk Park, Jina Park, Jee Hyun Kong, Ji Sun Nam, Chul Woo Ahn, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee, Soon Won Hong
-
J Korean Endocr Soc. 2006;21(1):53-57. Published online February 1, 2006
-
DOI: https://doi.org/10.3803/jkes.2006.21.1.53
-
-
 Abstract Abstract
 PDF PDF
- Acromegaly is a clinical syndrome, which is caused by an excess of growth hormone (GH), most commonly secreted from a pituitary solitary adenoma. However, our patient had bilateral GH-secreting pituitary tumors, the incidence of which has been reported in only 1.3 to 1.69% of all acromegalic patients. A 59-year-old female, with no family history of pituitary adenomas, demonstrated an increased level of serum insulin-like growth factor-1 (IGF-1), and GH not suppressed after 75 g oral glucose loading. On a preoperative MRI, only one pituitary tumor, measuring 1.1 x 0.7 cm, could be observed using sellar MRI. After surgical resection of the tumor, her headache and myalgia were sustained, and the IGF-1 level was still in a high titer. Therefore, a follow-up sellar MRI was taken, and a 0.6 x 0.7 cm sized newly growing pituitary tumor was found on the other side. With a retrospective review of radiological examinations, the patient was found to have bilateral tumors. The 0.3 cm sized tumor on the left was too small to be detected on the preoperative MRI. As the patient preferred medical treatment after surgery, she was treated with sandostatin analogues. Acromegaly with bilateral GH-secreting pituitary tumors, is a very rare disease, with no previous case having been reported in Korea. Herein, we report the case with a review of the literature.
- A Case of Acromegaly with Gall Bladder Cancer.
-
Ji Sun Nam, Chul Sik Kim, Jee Hyun Kong, Hai Jin Kim, Jin A Park, Jong Suk Park, Chul Woo Ahn, Se Joon Lee, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee
-
J Korean Endocr Soc. 2005;20(4):401-406. Published online August 1, 2005
-
DOI: https://doi.org/10.3803/jkes.2005.20.4.401
-
-
 Abstract Abstract
 PDF PDF
- Acromegaly is a systemic endocrine disorder due to an excessive release of growth hormone, which increases the serum levels of insulin-like growth factor-1(IGF-1). Elevated levels of these hormones are assumed to increase the incidence of malignant tumors in patients with acromegaly, due to by stimulating the growth and maturation of cells. In particular, IGF-1 is considered to be closely related with the development of colon polyps and colon cancers. Studies suggest that various malignant tumors, including thyroid cancer, brain tumor and renal cell carcinomas, are also more common in patients with acromegaly. Here, a case of gall bladder cancer in a patient with acromegaly, and the possible relationships between these two disorders, is reported.
- A Case of Hepatomegaly due to Diabetic Glycogenosis Reversed by Glycemic Control.
-
Jina Park, Dae Hoon Song, Jong Suk Park, Joo Young Nam, Chul Sik Kim, Dol Mi Kim, Chul Woo Ahn, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee, Hae Ryoung Kim, Chan Il Park
-
J Korean Endocr Soc. 2004;19(2):223-228. Published online April 1, 2004
-
-
-
 Abstract Abstract
 PDF PDF
- Diabetes mellitus is well known to be associated with various structural and functional liver abnormalities. If diabetic patients are accompanied by hepatomegaly or abnormal findings from a liver function test, the most common pathological findings are steatosis and glycogenosis. The steatosis is characterized by deposition of macrovesicular fat droplets in the hepatocytes, which is common in obese, type 2 diabetes mellitus. If macrovesicular steatosis is combined with mixed inflammatory infiltrate, without evidence of alcoholic hepatitis, the case could be diagnosed as nonalcoholic steatohepatitis (NASH). NASH has the possibility of progressing to cirrhosis. Secondary glycogenosis is common in uncontrolled type 1 diabetes mellitus, and is completely reversible. A 22-year-old male, with uncontrolled type 1 diabetes mellitus, was admitted with anorexia, nausea and right upper quadrant pain. Hepatomegaly and elevated aminotransferases were noted. He was diagnosed as diabetic glycogenosis using computed tomogram and liver biopsy. The hepato megaly and liver function test abnormalities were markedly improved with glycemic control
- Relationship with Serum Adiponectin Concentrations and Obesity in Korean Children.
-
Hyoun Ah Kim, Hyoung Suk Lee, Chul Sik Kim, Chul Woo Ahn, Yoon Sok Chung, Kwan Woo Lee, Kap Bum Huh, Dae Jung Kim
-
J Korean Endocr Soc. 2003;18(5):473-480. Published online October 1, 2003
-
-
-
 Abstract Abstract
 PDF PDF
- BACKGROUND
Adiponectin is an adipocytokine that is highly specific to adipose tissue. In contrast to other adipocytokine, the adiponectin levels are decreased in obesity and/or type 2 diabetes. There are few studies regarding the correlation between the adiponectin concentration and obesity in children. Thus, whether the serum adiponectin concentrations are associated with adiposity in children was investigated. METHODS: One hundred and sixty four subjects were selected from the participants in an ongoing study on the relationship between birth weight and insulin resistance in children. The current weights, heights, body fat percentages, waist circumferences, blood pressures, lipid profiles and insulin resistance, by the HOMA method, were measured in all the subjects. The serum adiponectin concentrations were determined by a validated sandwich ELISA, using a human adiponectin-specific antibody. RESULTS: The serum adiponectin concentration was negatively correlated with the body mass index, waist circumference, systolic blood pressure, insulin resistance by HOMA and serum triglycerides, and positively correlated with the serum HDL cholesterol level. The serum adiponectin concentrations in the boys were significantly lower than in the girls. In a multiple regression analysis, the serum adiponectin concentration was strongly associated with waist circumference and gender. CONCLUSION: It is concluded that there was an inverse relationship between the serum adiponectin concentration and abdominal adiposity in children. However, further studies on independent gender differences on adiponectin are needed.
- A Case of Riedel's Thyroiditis in a Patient with a History of Subacute Thyroiditis.
-
Chul Sik Kim, Sung Ju Lee, Jong Suk Park, Joo Young Nam, Dol Mi Kim, Chul Woo Ahn, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee
-
J Korean Endocr Soc. 2003;18(4):414-419. Published online August 1, 2003
-
-
-
 Abstract Abstract
 PDF PDF
- Riedel's thyroiditis is a rare form of chronic thyroiditis, characterized by a fibroinflammatory process which partially destroys the thyroid, often involving surrounding tissues. The relationship of Riedel's thyroiditis to other forms of thyroiditis is not clear. A case of Riedel's thyroiditis in a 51-year-old female patient, admitted with a previous diagnosis of subacute thyroiditis, is reported. She was first diagnosed with subacute thyroiditis based on clinical manifestation and radiologic and laboratory results. She was treated with glucocorticoid for 8 weeks. The follow-up lasted for 12 months. However, three years later she underwent a thyroidectomy operation due to an enlargement of the thyroid nodule and suspicion of malignancy. Histopathologic examination confirmed that she had Riedel's Thyroiditis. Until now, few case of Riedel's thyroiditis in patients with a history of subacute thyroiditis have been reported in the literature. Although the etiology of Riedel's thyroiditis is unknown, it may develop in the course of subacute thyroiditis.
|